Gout
by drdoc on-line
Gout is a syndrome caused by an inflammatory response to the formation of monosodium urate monohydrate crystals which develop secondary to hyperuricemia. Acute and chronic forms are recognized. Hyperuricemia may be due to environmental and/or genetic factors.
Clinical features Most commonly affects middle-aged males. It is an acute and usually relapsing self-limiting arthritis. A Chronic form associated with collections of crystals - tophus formation occurs, and bone and joint destruction can occur.
It is commonly associated with
Obesity
Heavy alcohol intake
Hypertension
Renal impairment
Diuretic use.
It especially involves the first metatarsophalangeal joints especially the big toe, heels, ankles and knees.
Gout has been called the ‘disease of kings’.
The term ‘gout’, is derived from Latin ‘gutter’ (a drop) which reflects the notion that gout resulted from a local instillation of malevolent humour. These concepts are well illustrated in paintings of persons afflicted with gout. It is also seen as a "disease of plenty - which is an incorrect generalization.
Hyperuricemia has been defined as a serum or plasma urate concentration greater than
7.0mg/dl (0.42mmol/l) in males
6.0mg/dl (0.36 mmol/l) in females
It is important to recognize the clear
distinction between hyperuricemia and gout.
Hyperuricemia is clearly a risk factor for the development of gout, the risk increasing with a higher urate concentration. However, many years of hyperuricemia have usually elapsed before the development of acute gouty arthritis, and in some hyperuricemic people gout may never develop.
Acute gout is characterized rapid onset of pain,
There is pain and the swelling, with associated redness of the affected joint. The pain may be excruciating. In over half of the initial attacks, the onset is in the first metatarsophalangeal joint (MTP), and in time, this joint is affected in some 90% of patients with gout.
Almost any joint can be affected. However, the
lower limbs are involved more often than upper limbs.
Mild attacks may resolve within one to two days. More
severe attacks exhibit rapidly increasing pain reaching its peak usually within
a few hours, remaining at this level for some one to three days, then slowly
remitting, such that the attack has often subsided within seven to ten days. It
may take several weeks before very severe attacks settle completely. Several
factors have been recognized as precipitants of acute attacks of gout.
These include:
Acute illness
Trauma
Surgery
Alcohol (especially beer and wines)
Drugs that either increase or decrease the plasma
urate concentration. ..especially diuretics
A radical change in diet or food binge
Patients who develop chronic gout usually are those
whose hyperuricemia is not controlled.
Tophi appearing within the first two years of gout are
extremely rare and patients have usually suffered from gout for at least 10
years before tophi develop. The tophi are collections of crystals that form
deposits in soft tissue, joint, bone and tendons. They cause erosion and
destruction of the bone, and cause damage that may lead to crippling. Such
crippling is I feel a tragedy, as this situation is completely controllable, and
preventable. To be crippled from gout is "completely unnecessary, and tragic".
Acute gout - swelling redness and heat in the joint
Chronic joint involvement with crystal accumulation - tophus]
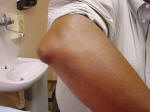
Early crystal accumulation at the elbow - tophus
Neglected chronic gout with tophi
Therapy for Gout Therapy in gout is
directed towards:
1. the management of acute attacks
2. The prevention of further attacks and the
complications of chronic gout.
It is important when considering therapy for gout to distinguish between therapy for reducing inflammation and that for managing hyperuricemia.
The decision to introduce drugs to normalize hyperuricemia depends in part :
1. on the number of previous attacks of acute gout
2. The degree of hyperuricemia
3. The presence or otherwise of reversible factors
4. The presence of tophi.
Urate lowering drugs will not normally be used
after just a single attack of gout. but should be considered after the second or
third attacks. Furthermore, they should virtually always be used for tophaceous
gout.
The patient needs to be informed that the decision to commence antihyperuricemic therapy usually implies life-long treatment and the patient, needs to be committed to this policy.
Therapy is aimed at controlling the acute attack -
completely, and then if indicated, controlling the uric acid level at source or
by increasing it's removal from the body. Introduction of these second line
drugs must never be during the actual acute attack, as they will potentially
aggravate the acute episode and prolong it.
Both increases and decreases in plasma urate
concentrations may precipitate or prolong an attack of gout. Therefore, therapy
aimed at reducing urate concentrations should be delayed until after the
complete resolution of all signs of inflammation. It must be noted that one of
the commonest cause of difficulty in controlling an attack, is the simultaneous
administration or withdrawal of drugs that alter the plasma urate concentration.
Acute Gout
Colchicine and Nonsteroidal anti-inflammatory drugs
(NSAIDs) are effective in the treatment of acute gout and are much superior to
paracetamol or aspirin. In addition, NSAIDs are superior to colchicine in terms
of speed of onset of action. Thus, despite having been used for centuries,
colchicine is usually reserved for patients in whom NSAIDs are
contraindicated. Oral corticosteroids such as prednisone is useful in resistant
gout and we use this for 10 days to 2 weeks, during and after treatment of the
acute episode, whilst instituting second line therapy to prevent recurrence in
patients who are difficult to control.
Intra-articular administration of Corticosteroids is a
particularly effective means of terminating an attack of gout.
Resolution is typically complete within 12–24 hours.
Cortisone is of particular value in some patients with
renal impairment and other conditions where the use of full doses of other drugs
may be relatively contraindicated.
Recurrent Gout
Despite the use of effective prophylaxis, only
correction of the hyperuricemia can alter the underlying tendency to gout.
Drugs to correct hyperuricemia act either by
Promoting the renal excretion of urate - (uricosuric
agents) or by
Decreasing urate production - by inhibiting xanthine
oxidase (allopurinol)
Unfortunately allergy to allopurinol is possible.
Hypertension also can occur with allopurinol, so your doctor should check your blood pressure after starting it.
If allopurinol is not tolerated because of allergy,
probenecid can be used.
It cannot be stressed too much that antihyperuricemic
drugs should not be commenced until an attack of gout has settled completely.
In addition, I use prophylactic doses of colchicine
or NSAID's or even low dose cortisone to minimize the risk of inducing an attack
of acute gout, whilst introducing the second line - preventative drugs..
Tophaceous Gout
The principle of treatment of tophi is to lower the
plasma urate concentration to such a degree, as to allow urate to be resorbed
from the surface of the tophi. The uric acid therefore is slowly excreted
at the kidney, and production is lower than excretion, resulting in net loss of
uric acid.
(In this phase, I use citrosoda 10ml twice a day to
prevent deposition of crystal in the kidney, and prevent kidney stone
developement.) It is therefore aimed at maintaining the urate concentration
within the middle of the optimal range.
This requires the long-term use of urate-lowering
drugs over many years.
Colchicine and most NSAIDs, while controlling acute
attacks, will not prevent the formation of tophi and may, by preventing the
inflammatory response, actually increase the development of tophi unless
hyperuricemia is controlled at the same time.
Gout and diet
General Guidelines for Gout prevention
Avoid purine-rich foods (see Diet sheet chart - below
)
The higher the purine content, the more uric acid will
be produced in the body.
If you are overweight, try and achieve your ideal
weight through slow, controlled weight loss (maximum 500 g per week).
Rapid / sudden fasting is not recommended as this can
raise uric acid levels and aggravate gout.
Avoid heavy, rich meals with high fat and protein
content.
Alcohol should be avoided, particularly wine since it
interferes with uric acid excretion.
I generally require patients to comply strictly with diet whilst starting them on second line medication therapy for gout, but liberalize the diet after approximately six weeks, once stable.
Diet sheet
Forbidden
Very high purine content.
Herring, herring roe, meat extracts, mussels,
Sardines, yeast (brewer’s and baker’s).
Alcohol : Alcohol contains no purine but interferes
with uric acid excretion.
Liver
Avoid
High purine content - not more than one item
once a week.
Anchovies, bacon, chicken soup, Beef, mutton leg,
mutton chop, pheasant, salmon, sausage, trout, turkey, veal, venison, lobster,
crab.
Moderation
Moderate purine content-not more than one item 4 times
a week.
Asparagus, bass, bouillon, brains, cauliflower,
chicken, duck, halibut, ham, kidney beans, lentils, Lima beans, liverwurst,
mushrooms, oysters, peas, plaice, pork, rabbit, roe, shad, spinach, tongue,
tripe, tuna, wholegrain cereals and bread.
Acceptable
Low or no purine content - as often as desired.
Beverages -tea, coffee, cocoa, chocolate
Carbonated soft drinks
Fruit juices
Sugar, sweets
Vegetables : (except those under BE CAREFUL)
Vegetables and cream soups (no meat stock)
Butter, fats of all kinds (in moderation)
Bread (except wholegrain)
Cereals (except wholegrain)
Cheese : all kinds (in moderation)
Eggs
Fruit
Milk - buttermilk, condensed, malted
Nuts - all kinds, peanut butter Drink plenty of water
(2-3 litres per day) to help flush uric acid through the kidneys. Please note -
if you have cardiac or kidney disease, your doctor may actually require fluid
restriction - and you should consult him regarding fluid intake allowance.
Keep dietary fat to a minimum.
ESSENTIAL - Take your prescribed medication regularly.